Intraocular injections, also referred to as “shots” by patients, is an innovative method of treatment for retinal diseases. Intraocular injections have been commonly used since 2006, when a medicine called Avastin was first introduced into the field of ophthalmology. It is a highly effective treatment, which allows to prevent blindness even in patients with advanced diseases. The main disadvantage of this solution is that, at this stage, there is no medication that works “once and for ever”. Injections have to be repeated.
Dr Agnieszka Nowosielska was among the first ophthalmologists in Poland to start performing intravitreal injections in the course of neovascular AMD back in 2006. Since then, she has performed more than 11 000 intraocular injections of different medicines (Avastin, Triamcynolon, Lucentis, Eylea medicine and Ozurdex implant). Dr Nowosielska successfully treats patients with neovascular AMD, diabetic macular oedema or neovascular glaucoma by means of intraocular injections. Her broad clinical experience enabled her to develop an innovative administration regime of medication for AMD. Anti-VEGF treatment proposed by dr Nowosielska is highly effective. It consists of establishing an adequate dose of medicine for every patient depending on his or her individual needs in order to achieve the best results, that is to restore the visual acuity, with as few injections as possible.
What are intraocular injections? What types of injections are used in ophthalmology? What eye diseases are treated with intraocular injections?
Intraocular injections, which can be defined as shorts of medicines into the eye, is an innovative method of treatment for eye diseases. It allows to administer the medicine directly to the place where it is needed, thus avoiding the necessity of introducing the medicine into the whole system and dealing with all the related complications. Different medicines are used in ophthalmology. In diseases such as neovascular AMD, diabetes or retinal vein occlusions, anti-VEGF (anti-vascular endothelial growth factor) medication is administrated. In diabetes, retinal vein occlusions and uveitis (inflammation of the middle layer of the eye), steroids are used together with anti-VEGF medication. In bacterial uveitis, on the other hand, it is necessary to administer antibiotics. On occasions, injections are the only method of treatment, but in some cases, they have to be combined with other forms of therapy.
What is anti-VEGF treatment? What does anti-VEGF treatment consist of? What medicines are used in anti-VEGF treatment?
Anti-VEGF treatment consists of administrating anti-VEGF medication into the eyeball. Anti-VEGF stands for anti-vascular endothelial growth factor – a substance that blocks vascular endothelial growth factor. Avastin (bevacizumab) was the first medicine of this group. It was registered by FDA (Food and Drug Administration – an institution that authorizes placing on the market medicines and food in the United States) as a medicine administrated intravenously and indicated to treat cancer of the colon. Avastin is indicated to treat cancer, because, like other anti-VEGF medication, it blocks the growth of new blood vessels, thus preventing cancer from growing due to the lack of blood supply. Similarly, when the growth of new blood vessels is blocked, diseases such as neovascular AMD cannot develop. Research has demonstrated that in neovascular AMD, diabetic macular oedema or macular oedema in the course of retinal vein occlusion, the level of VEGF in the eye is raised. This is the reason why anti-VEGF medication is used to treat these diseases. Currently, it is the most common method of treatment. When talking about intraocular injections, patients usually refer to anti-VEGF medication. There are three anti-VEGF medicines used in the treatment for neovascular AMD available on the market. They include: Avastin (bevacizumab), Lucentis (ranibizumabum) and Eylea (aflibercept). In anti-VEGF treatment, the outset of the treatment as well as the frequency of drugs administration are of vital importance. An inadequate regime of treatment may lead to its ineffectiveness.
Which medicine should be chosen: Avastin, Lucentis or Eylea? What are the differences between Avastin, Lucentin and Eylea?
As it was previously mentioned, Avastin (bevaxizumab) was the first anti-VEGF medication registered in the world. It has been used in ophthalmology since the turn of the years 2005 and 2006. Philip Rosenfeld from Badcom Palmer University in Florida was the first person who thought that Avastin could be used in the treatment for neovascular AMD. He correctly assumed that if Avastin could stop the growth of cancerous tumour by blocking the growth of its blood vessels, it could be as effective in the case of neovascular AMD, a disease caused by the uncontrolled growth of new blood vessels underneath the retina.
The first attempts to use Avastin consisted in administrating intravenously the same dose that was used in oncology. Currently, a significantly reduced dose (4000 times smaller) is used and administrated directly into the eye instead of into the vein. This prevents patient from suffering from adverse events. Avastin is owned by the company Genentech.
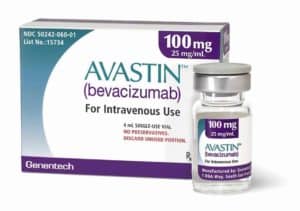
Source: Genentech
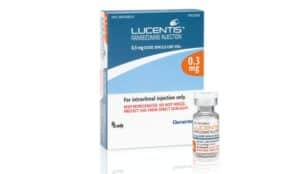
Lucentis was especially designed and registered to treat wet AMD. From the chemical point of view, it is a derivative of Avastin. It was produced by Genentech, because after the success of Avastin, the company wanted to introduce a medicine developed specifically for ophthalmic use. The mechanism of action and adverse events of Lucentis and Avastin are similar. Clinical trials CATT/IVAN have demonstrated that the effectiveness of Avastin and Lucentis is also akin. The same applies to the adverse events. The effectiveness of treatments is usually related to the regime of treatment and the experience of the doctor who performs it.
Eylea is the most recent medicine that we use to treat wet AMD. Eylea is produced by Bayer. It is also a cancer medicine, which was tried out in ophthalmology. It turned out that it achieved very good results in retinal oedema and neovascular AMD. The mechanism of action of Eylea is slightly different from Avastin or Lucentis and some patients react better to the treatment.
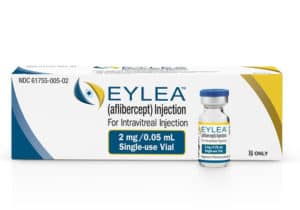
Source: Regeneron
Individual sensitivity to these medicines may vary from patient to patient. According to clinical trials of these medicines, they act similarly.
What does steroid treatment consist of? What eye diseases are treated with steroids? Are steroids safe?
Steroids are widely used in medicine due to their strong anti-inflammatory and anti-swelling properties. They also block the process of cell division. Currently, in ophthalmology, steroids are mainly administrated locally (that is, exactly where they are needed) in order to achieve better medical results and avoid systemic complications. Generally, steroids are administrated if the defects in the eye are caused by systemic changes. It is because steroids have been reported to have numerous adverse events, such as diabetes, gastric ulcers or mood disorders.
Steroids act differently than anti-VEGF medication and, therefore, they are indicated to treat diseases in which anti-VEGF medication fails to deliver the expected results or is less effective. For example, steroids are not an effective method of treatment for AMD. Anti-VEGF medication remains the only available method of treatment for AMD.
The eye diseases that can be treated with steroids include uveitis (inflammation of the middle layer of the eye), diabetic macular oedema and retinal vein occlusion. Triamcinolone, Ozurdex and Illuvien are among the most common medicines from this group. All steroids have similar, local adverse events. They include glaucoma and cataract. Secondary glaucoma (raised eye pressure) occurs in 25-30% of the cases, in which steroids are administrated into the eye. Raised eye pressure is usually temporary; it drops once an adequate medicine is administrated. A very small proportion of patients requires glaucoma surgery. Steroids may also speed up the process of cataract progression. However, it should be remembered that steroids are often used to treat uveitis or diabetes and these are the diseases that may speed up the process of cataract progression themselves. For that reason, cataract is considered to be an unpleasant, but easy to remove complication. If steroids are used in patients after cataract surgery, such problem does not exist.
What steroids are used in ophthalmology?
Triamcynolon is a derivative of prednizolon. Triamcinolone has strong anti-inflammatory and anti-swelling action and blocks the process of cell division. In ophthalmology, it was among the first medicines to be administrated directly into the eye. It is administrated into the eye “off label” (for an unapproved route of administration), because it is registered as a medicine to be administrated intramuscularly. It is a very cheap and effective medicine. Its effects in the eye can last for about 4-6 months. Following this period, treatment usually has to be repeated. Triamcinolone is administrated into the eye in the form of suspension, so dark floaters may appear in the visual field during the first days after the injection. They disappear after a few days.
Ozurdex is a derivate of dexamethazon. It is an implant designed especially to be injected into the eye. It looks like a piece of white pencil load. Unlike Triamcinolone, it does not cause floaters in the visual field after the injection. Its effects in the eye can last for about 4-6 months.
Illuvien is another implant with steroid medicine registered to inject into the eye. It has been originally created for patients with uveitis, but it can also be used to treat diabetic macular oedema. Its effects in the eye can lasts even up to 2 years! That is why it is very convenient in application. In Poland it is barely used.
How does injection proceed?
Before the injection is performed, anaesthetic eye-drops or gel are administrated into the eye, depending on the preferences of the surgeon or the patient. The eye must be disinfected so that no bacteria are introduced into the eye during the injection. Then, the injection is performed. The surgeon performs it into a safe place in the eye, so that no eye structures get damaged.
Are intraocular injections safe? Are there any complications related to intraocular injections?
Intraocular injections are a safe procedure. They usually have little complications that can be divided into the local ones and the systemic ones. Local complications do not vary, because they are a consequence of introducing a needle inside the eye. They may include: subconjunctival haemorrhage (red eye), eye pinching, eye stinging, foreign-body sensation or seeing black spots. These symptoms are not dangerous. They regress after a few days. Attention should be given to the dry eye syndrome – a symptom that often occurs as a result of a long-term treatment. If injections, disinfection and anaesthesia procedures are repeated frequently, the eye may be irritated, thus becoming permanently sensitive to light and wind. Pinching and stinging may also be experienced. Unfortunately, patients who are treated with this method have to be prepared for those events. However, there are ways to deal with them, for example, using moisturizing eye-drops (ideally without preservatives), such as Hylocomod, Hyloparin, Hyal-eye, Thealoz Duo, Systane, Cornegel, among others.
Eyeball inflammation is the most serious complication. It is a very rare complication, but if it appears it can be really dangerous and requires an immediate treatment. Therefore, if a sudden eye pain and vision deterioration occur after the injection, it is vital to contact the ophthalmologist who performed the injection as soon as possible. Systemic complications, that affect the whole body, can also be distinguished. All anti-VEGF medications (Avastin, Lucentis, Eylea) have a similar general effect and cannot be divided into “better” and “worse”. The most severe complications include stroke, heart attack or varicose veins, which are due to the increase of the number of blood clots in the system. The risk of suffering from any of these diseases after administrating anti-VEGF medication has been estimated at around 1%. However, it should be noted that the majority of patients with neovascular AMD or diabetes taking anti-VEGF medication is subject to a higher risk of cardiovascular diseases or they have already experienced such episodes.
Does intraocular injections hurt?
Injections are completely painless, as they are performed under local anaesthesia. However, some patients get nervous, because they are aware of what the injection consists of. In such a case, it is advisable to take a sedative before the procedure.
Am I going to restore normal vision after the injection?
Just after the injection, vision is always worse due to the disinfection procedure itself and the action of eye dilating eye-drops. However, worse vision lasts only for about a few hours. On the first day after the injection, some patients may see black dots or specks. These symptoms usually disappear after one day and they are not dangerous.
Are there any contraindications for intraocular injection?
The main contraindication for performing intraocular injection is a bacterial infection of the eye surface. In such a case, there is a risk of spreading the inflection to the inside of the eye, which may be dangerous. According to some physicians, it is not recommended to perform injections shortly after a stroke or a heart attack and it is necessary to wait six months of their occurrence, because there is a risk of suffering from another episode of that kind. Unfortunately, the truth is that a stroke or a heart attack increases the risk of further incidents in the same patient. Therefore, it is vital to eliminate the risk related to poor circulation and to take medicines lowering blood clotting. When in doubt, it is always recommended to consider the whole clinical picture and the specific case. It should also be noted that in some cases, waiting six months for an ophthalmic treatment may lead to a complete blindness in some patients. These are very hard decisions, especially because every specialist assesses the patient’s situation based on his or her own experience. Patients with neovascular AMD, who receive a long-term treatment with anti-VEGF medication, should take medicines lowering blood clotting permanently (unless retinal haemorrhage occurs).
FAQ
Intraocular injections, which can be defined as shorts of medicines into the eye, is an innovative method of treatment for eye diseases. It allows to administer the medicine directly to the place where it is needed, thus avoiding the necessity of introducing the medicine into the whole system and dealing with all the related complications. Different medicines are used in ophthalmology. In diseases such as neovascular AMD, diabetes or retinal vein occlusions, anti-VEGF (anti-vascular endothelial growth factor) medication is administrated. In diabetes, retinal vein occlusions and uveitis (inflammation of the middle layer of the eye), steroids are used together with anti-VEGF medication. In bacterial uveitis, on the other hand, it is necessary to administer antibiotics. On occasions, injections are the only method of treatment, but in some cases, they have to be combined with other forms of therapy.
Anti-VEGF treatment consists of administrating anti-VEGF medication into the eyeball. Anti-VEGF stands for anti-vascular endothelial growth factor – a substance that blocks vascular endothelial growth factor. Avastin (bevacizumab) was the first medicine of this group. It was registered by FDA (Food and Drug Administration – an institution that authorizes placing on the market medicines and food in the United States) as a medicine administrated intravenously and indicated to treat cancer of the colon. Avastin is indicated to treat cancer, because, like other anti-VEGF medication, it blocks the growth of new blood vessels, thus preventing cancer from growing due to the lack of blood supply. Similarly, when the growth of new blood vessels is blocked, diseases such as neovascular AMD cannot develop. Research has demonstrated that in neovascular AMD, diabetic macular oedema or macular oedema in the course of retinal vein occlusion, the level of VEGF in the eye is raised. This is the reason why anti-VEGF medication is used to treat these diseases. Currently, it is the most common method of treatment. When talking about intraocular injections, patients usually refer to anti-VEGF medication. There are three anti-VEGF medicines used in the treatment for neovascular AMD available on the market. They include: Avastin (bevacizumab), Lucentis (ranibizumabum) and Eylea (aflibercept). In anti-VEGF treatment, the outset of the treatment as well as the frequency of drugs administration are of vital importance. An inadequate regime of treatment may lead to its ineffectiveness.
As it was previously mentioned, Avastin (bevaxizumab) was the first anti-VEGF medication registered in the world. It has been used in ophthalmology since the turn of the years 2005 and 2006. Philip Rosenfeld from Badcom Palmer University in Florida was the first person who thought that Avastin could be used in the treatment for neovascular AMD. He correctly assumed that if Avastin could stop the growth of cancerous tumour by blocking the growth of its blood vessels, it could be as effective in the case of neovascular AMD, a disease caused by the uncontrolled growth of new blood vessels underneath the retina.
The first attempts to use Avastin consisted in administrating intravenously the same dose that was used in oncology. Currently, a significantly reduced dose (4000 times smaller) is used and administrated directly into the eye instead of into the vein. This prevents patient from suffering from adverse events. Avastin is owned by the company Genentech.
Lucentis was especially designed and registered to treat wet AMD. From the chemical point of view, it is a derivative of Avastin. It was produced by Genentech, because after the success of Avastin, the company wanted to introduce a medicine developed specifically for ophthalmic use. The mechanism of action and adverse events of Lucentis and Avastin are similar. Clinical trials CATT/IVAN have demonstrated that the effectiveness of Avastin and Lucentis is also akin. The same applies to the adverse events. The effectiveness of treatments is usually related to the regime of treatment and the experience of the doctor who performs it.
Eylea is the most recent medicine that we use to treat wet AMD. Eylea is produced by Bayer. It is also a cancer medicine, which was tried out in ophthalmology. It turned out that it achieved very good results in retinal oedema and neovascular AMD. The mechanism of action of Eylea is slightly different from Avastin or Lucentis and some patients react better to the treatment.
Individual sensitivity to these medicines may vary from patient to patient. According to clinical trials of these medicines, they act similarly.
Steroids are widely used in medicine due to their strong anti-inflammatory and anti-swelling properties. They also block the process of cell division. Currently, in ophthalmology, steroids are mainly administrated locally (that is, exactly where they are needed) in order to achieve better medical results and avoid systemic complications. Generally, steroids are administrated if the defects in the eye are caused by systemic changes. It is because steroids have been reported to have numerous adverse events, such as diabetes, gastric ulcers or mood disorders.
Steroids act differently than anti-VEGF medication and, therefore, they are indicated to treat diseases in which anti-VEGF medication fails to deliver the expected results or is less effective. For example, steroids are not an effective method of treatment for AMD. Anti-VEGF medication remains the only available method of treatment for AMD.
The eye diseases that can be treated with steroids include uveitis (inflammation of the middle layer of the eye), diabetic macular oedema and retinal vein occlusion. Triamcinolone, Ozurdex and Illuvien are among the most common medicines from this group. All steroids have similar, local adverse events. They include glaucoma and cataract. Secondary glaucoma (raised eye pressure) occurs in 25-30% of the cases, in which steroids are administrated into the eye. Raised eye pressure is usually temporary; it drops once an adequate medicine is administrated. A very small proportion of patients requires glaucoma surgery. Steroids may also speed up the process of cataract progression. However, it should be remembered that steroids are often used to treat uveitis or diabetes and these are the diseases that may speed up the process of cataract progression themselves. For that reason, cataract is considered to be an unpleasant, but easy to remove complication. If steroids are used in patients after cataract surgery, such problem does not exist.
Triamcinolone is a derivative of prednizolon. Triamcinolone has strong anti-inflammatory and anti-swelling action and blocks the process of cell division. In ophthalmology, it was among the first medicines to be administrated directly into the eye. It is administrated into the eye "off label" (for an unapproved route of administration), because it is registered as a medicine to be administrated intramuscularly. It is a very cheap and effective medicine. Its effects in the eye can last for about 4-6 months. Following this period, treatment usually has to be repeated. Triamcinolone is administrated into the eye in the form of suspension, so dark floaters may appear in the visual field during the first days after the injection. They disappear after a few days.
Ozurdex is a derivate of dexamethazon. It is an implant designed especially to be injected into the eye. It looks like a piece of white pencil load. Unlike Triamcinolone, it does not cause floaters in the visual field after the injection. Its effects in the eye can last for about 4-6 months.
Illuvien is another implant with steroid medicine registered to inject into the eye. It has been originally created for patients with uveitis, but it can also be used to treat diabetic macular oedema. Its effects in the eye can lasts even up to 2 years! That is why it is very convenient in application. In Poland it is barely used.
Before the injection is performed, anaesthetic eye-drops or gel are administrated into the eye, depending on the preferences of the surgeon or the patient. The eye must be disinfected so that no bacteria are introduced into the eye during the injection. Then, the injection is performed. The surgeon performs it into a safe place in the eye, so that no eye structures get damaged.
Intraocular injections are a safe procedure. They usually have little complications that can be divided into the local ones and the systemic ones. Local complications do not vary, because they are a consequence of introducing a needle inside the eye. They may include: subconjunctival haemorrhage (red eye), eye pinching, eye stinging, foreign-body sensation or seeing black spots. These symptoms are not dangerous. They regress after a few days. Attention should be given to the dry eye syndrome – a symptom that often occurs as a result of a long-term treatment. If injections, disinfection and anaesthesia procedures are repeated frequently, the eye may be irritated, thus becoming permanently sensitive to light and wind. Pinching and stinging may also be experienced. Unfortunately, patients who are treated with this method have to be prepared for those events. However, there are ways to deal with them, for example, using moisturizing eye-drops (ideally without preservatives), such as Hylocomod, Hyloparin, Hyal-eye, Thealoz Duo, Systane, Cornegel, among others.
Eyeball inflammation is the most serious complication. It is a very rare complication, but if it appears it can be really dangerous and requires an immediate treatment. Therefore, if a sudden eye pain and vision deterioration occur after the injection, it is vital to contact the ophthalmologist who performed the injection as soon as possible. Systemic complications, that affect the whole body, can also be distinguished. All anti-VEGF medications (Avastin, Lucentis, Eylea) have a similar general effect and cannot be divided into "better" and "worse". The most severe complications include stroke, heart attack or varicose veins, which are due to the increase of the number of blood clots in the system. The risk of suffering from any of these diseases after administrating anti-VEGF medication has been estimated at around 1%. However, it should be noted that the majority of patients with neovascular AMD or diabetes taking anti-VEGF medication is subject to a higher risk of cardiovascular diseases or they have already experienced such episodes.
Injections are completely painless, as they are performed under local anaesthesia. However, some patients get nervous, because they are aware of what the injection consists of. In such a case, it is advisable to take a sedative before the procedure.
Just after the injection, vision is always worse due to the disinfection procedure itself and the action of eye dilating eye-drops. However, worse vision lasts only for about a few hours. On the first day after the injection, some patients may see black dots or specks. These symptoms usually disappear after one day and they are not dangerous.
The main contraindication for performing intraocular injection is a bacterial infection of the eye surface. In such a case, there is a risk of spreading the inflection to the inside of the eye, which may be dangerous. According to some physicians, it is not recommended to perform injections shortly after a stroke or a heart attack and it is necessary to wait six months of their occurrence, because there is a risk of suffering from another episode of that kind. Unfortunately, the truth is that a stroke or a heart attack increases the risk of further incidents in the same patient. Therefore, it is vital to eliminate the risk related to poor circulation and to take medicines lowering blood clotting. When in doubt, it is always recommended to consider the whole clinical picture and the specific case. It should also be noted that in some cases, waiting six months for an ophthalmic treatment may lead to a complete blindness in some patients. These are very hard decisions, especially because every specialist assesses the patient's situation based on his or her own experience. Patients with neovascular AMD, who receive a long-term treatment with anti-VEGF medication, should take medicines lowering blood clotting permanently (unless retinal haemorrhage occurs).
The eye does not require any special care after an intraocular injection. It is important to be careful so as the eye does not get infected.
No special preparation is needed before performing an intraocular injection. On the day of the injection, it is necessary to follow the daily care routine, have breakfast and take the medication that is taken on a daily basis. Medication lowering blood clotting should not be discontinued.
No important activities should be planned on the day of the injection, because it is difficult to predict how the patient would feel. Patients who receive injections regularly normally know whether their vision after the injection allows them to carry out their daily activities or not.
 Nagłe przypadki
Nagłe przypadki